Occupational therapy: how all work and more play restores some “normal” to childhood
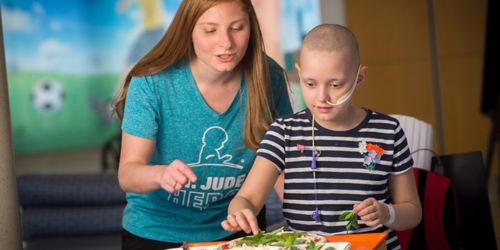
Zoe Oliver puts the finishing touches on her “dream pizza” with encouragement from her occupational therapist, Sarah Schwartzberg, MSOT, OTR/L.
Zoe Oliver stands up at a food prep table near the Kay Kafe pizza kitchen at St. Jude Children’s Research Hospital and recites all the steps for her “dream pizza” recipe. Next, she methodically rips fresh basil leaves in half until she has filled a small bowl with this key ingredient. Finally, Zoe layers thick tomato sauce and cheese on a fresh crust and tops them with the fragrant basil. This may sound like fun, but preparing a favorite dish is also part of the rehabilitation process for our patients at St. Jude. In fact, each of those three tasks is a separate mode of therapy that helps Zoe return to a normal life after undergoing a stem-cell (bone marrow) transplant for leukemia.
This is a great example of how my team members in St. Jude Occupational Therapy find engaging ways to help kids develop or regain the strength, coordination and skills they need to do the activities and tasks (occupations) that are important to them.
How can making a pizza develop strength and coordination?
Layering three toppings on a small pizza may seem like a light task, but not if you can’t stand up for very long or coordinate your movements to grasp the toppings or even see where your ingredients are kept.
Sarah Schwartzberg, Zoe’s occupational therapist, began planning how to help the high-spirited nine-year-old from Charlotte, North Carolina, regain a variety of life skills several weeks after she underwent her transplant. Preparing food was one of the focus areas because Zoe really enjoys cooking with her dad.
“Food prep work is an instrumental activity of daily living and I want Zoe to have the strength, fine motor skills and endurance to participate in this task,” Sarah explains. “She also felt as though her memory was not as strong as it once was, and having her state the food prep directions out loud helped her to work on sequencing a task.”
While Zoe was cheerfully tearing basil leaves in half, she was developing her dexterity or fine motor skills. These hand movements allow individuals to participate in everyday tasks ranging in complexity from completing a puzzle, to playing video games, to taking notes at school.
Watch occupational therapists Dr. Jessica Sparrow and Jordan Shoup, a former occupational therapy student, combine yoga with story-telling to help a 5-year-old brain cancer patient regain strength and coordination.
Why does a pediatric cancer center provide occupational therapy?
Occupational therapy has recently emerged as a rehabilitative service for pediatric oncology. My group is part of St. Jude Rehabilitation Services, which also includes teams of physical therapists, speech-language pathologists and audiologists.
Young cancer patients need this type of care because both cancer and its medical treatments take away a lot of the “normal” from their lives, such as a neurosurgery patient who has a difficult time moving or coordinating his hands after a brain tumor has been removed.
Aside from the direct disruptions from disease and treatment, a young cancer patient’s life is also affected by spending time away from home and not interacting with their friends, classmates and siblings. This separation can restrict the child’s ability to grow and learn.
For a specific example of how occupational therapy complements pediatric cancer treatment, we treat a chemotherapy side-effect called peripheral neuropathy, which causes significant weakness and a lack of sensation in the feet and hands. Many every-day tasks can become difficult for a patient with this syndrome, from squeezing toothpaste onto a toothbrush, to opening a container or texting with friends. While we wait for the affected nerves to heal, an occupational therapist can apply orthotic devices (splints and supports) and adaptive techniques—tricks and tools for improving hand movement.
And for a child who's lost her vision from retinoblastoma or a neurological impairment, we help them learn new skills or relearn old skills. For one child who lost her eyesight to cancer, our therapists designed adaptive strategies for her to once again play Connect4 with her siblings.
For both in-patient and outpatient care, our young patients have a lot of fun while working very hard to build skills to become as independent as possible.






